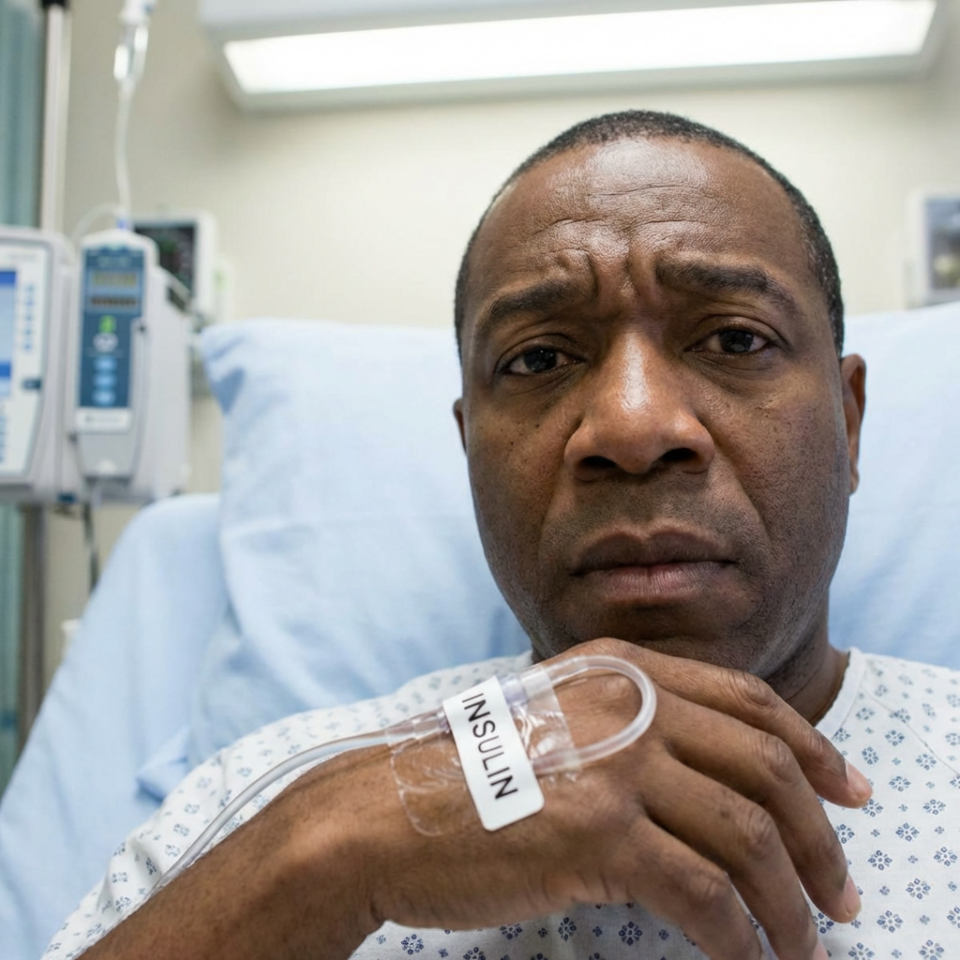
Diabetes is often framed as either Type 1 or Type 2. But for many patients—particularly in Black communities—that binary framework misses an important and potentially dangerous condition: Flatbush diabetes, also known as ketosis-prone diabetes (KPD).
First identified in the 1980s among African American patients in the Flatbush neighborhood of Brooklyn, this form of diabetes continues to be under-recognized, even by healthcare professionals.
What Is Flatbush Diabetes?
Flatbush diabetes is a hybrid form of diabetes that shares features of both Type 1 and Type 2 diabetes. Like Type 1 diabetes, patients often present suddenly with diabetic ketoacidosis (DKA)—a life-threatening condition. Like Type 2 diabetes, many patients can eventually come off insulin and maintain control with oral medications or lifestyle changes.
This dual nature is what makes it dangerous—and frequently misdiagnosed.
Flatbush diabetes disproportionately affects:
- African Americans
- Afro-Caribbean populations
- Hispanic populations
It is now recognized globally but remains especially relevant in populations with higher rates of Type 2 diabetes and health disparities.
For many physicians, this condition represents a critical diagnostic blind spot. They simply don’t think of the diagnosis.
The Clinical Presentation: A Dangerous First Impression
Patients with Flatbush diabetes often present with:
- Very high blood glucose levels
- Dehydration
- Nausea, vomiting, abdominal pain
- Confusion or altered mental status
- Diabetic ketoacidosis (DKA)
This presentation mimics classic Type 1 (insulin-dependent) diabetes, leading many doctors to assume lifelong insulin dependence. However, this assumption is often incorrect.
What Makes Flatbush Diabetes Different?
Flatbush diabetes has several defining features:
1. No Autoimmune Destruction
Unlike Type 1 diabetes, patients lack autoimmune markers such as GAD antibodies.
2. Reversible Insulin Deficiency
At diagnosis, insulin production appears severely impaired—but this is often temporary.
3. Potential for Remission
With proper treatment:
- Beta-cell function can recover
- Insulin may be discontinued within weeks to months
- Long-term management resembles Type 2 diabetes
This “reversible phase” is a hallmark of the condition.
Why Misdiagnosis Happens
Flatbush diabetes sits in a gray zone:
| Feature | Type 1 | Type 2 | Flatbush |
| DKA at onset | Yes | Rare | Yes |
| Autoantibodies | Present | Absent | Absent |
| Insulin dependence | Lifelong | Sometimes | Often temporary |
Because of this overlap, patients are frequently:
- Misclassified as Type 1
- Kept on unnecessary lifelong insulin
- Not counseled on remission potential
Implications for Black Health
Flatbush diabetes is more than a clinical curiosity—it is a health equity issue.
In communities with already high diabetes rates, delayed diagnosis and restricted access to specialty care can result in misdiagnosis. This leads to:
- Overtreatment or undertreatment
- Increased healthcare costs
- Poorer long-term outcomes
Recognizing Flatbush diabetes enables precision medicine for populations that need it most.
Treatment Approach
Acute Phase (Emergency)
- Treat DKA aggressively with insulin, fluids, and electrolytes
- Stabilize the patient (same as Type 1 DKA protocols)
- Allow a recovery phase
- Reassess insulin needs frequently
- Evaluate C-peptide and autoantibodies
- Gradually taper insulin if appropriate
Long-Term Management
- Lifestyle intervention (nutrition, physical activity)
- Oral agents (e.g., metformin)
- Ongoing monitoring for relapses
Many patients achieve insulin independence (go off insulin), though continued follow-up is essential.
What Clinicians Need to Do Differently
Think beyond just Type 1 vs. Type 2 tests for autoantibodies and beta-cell function. Reevaluate insulin dependence over time. Educate patients about the possibility of remission.
Final Thoughts
Flatbush diabetes challenges our understanding of how to classify diabetes. It reminds us that not all diabetes fits neatly into categories—and failing to recognize that can cost lives. For clinicians serving Black populations, awareness of Flatbush diabetes is not optional—it is essential.